Table of Contents
Hernias can be a source of discomfort and concern for many individuals, necessitating surgical intervention for resolution. The two primary surgical approaches for hernia repair are laparoscopic and open surgery for hernia. Both techniques have their unique characteristics, benefits, and potential drawbacks.
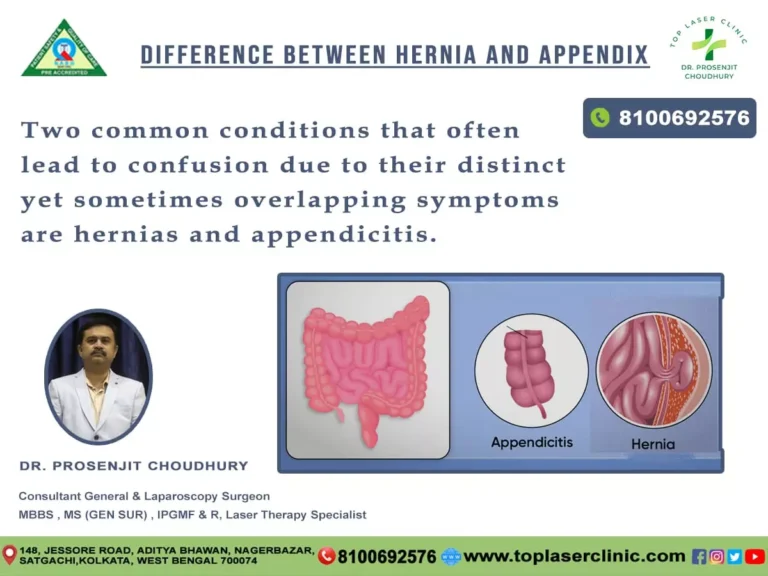
Understanding Hernias
This article aims to delve into the distinctions between laparoscopic and open surgery for hernia repair, helping individuals gain a comprehensive understanding of these procedures.
Before discussing the surgical procedures, it’s essential to comprehend what a hernia is. A hernia occurs when an internal organ or tissue pushes through a weak spot in the surrounding muscle or connective tissue, creating a bulge. Common types include inguinal (groin), umbilical (belly button), and incisional (resulting from a previous surgical incision) hernias.
Open Surgery for Hernia Repair
Open surgery has been the traditional method for repairing hernias. In this approach, the surgeon makes an incision directly over the hernia and pushes the protruding tissue back into place. The weakened muscle wall is then strengthened and reinforced with stitches or surgical mesh.
Open surgery provides the surgeon with direct access to the affected area, allowing for clear visibility and manual dexterity during the repair process.
Advantages of Open Surgery
- Accessibility: Surgeons have direct and clear access to the herniated area, enabling better visualization and manipulation of tissues.
- Versatility: This technique can be employed for various hernia types and sizes.
- Cost-Effective: Open surgery generally tends to be less expensive than laparoscopic procedures.
Disadvantages of Open Surgery
- Larger Incision: This technique involves a more significant incision, potentially leading to more postoperative pain and longer recovery times.
- Higher Risk of Complications: Due to the larger incision, there is a slightly higher risk of infection, blood loss, and a longer hospital stay.

Laparoscopic Surgery for Hernia Repair
Laparoscopic surgery, a more minimally invasive approach, involves making several small incisions through which a tiny camera (laparoscope) and specialized surgical tools are inserted.
The surgeon views the internal structures on a monitor and performs the repair using these instruments. The weakened muscle is reinforced with a synthetic mesh, similar to open surgery.
Advantages of Laparoscopic Surgery
- Minimal Scarring: The smaller incisions result in less visible scarring and potentially reduced postoperative pain.
- Faster Recovery: Patients often experience a quicker recovery time and can return to regular activities sooner than with open surgery.
- Reduced Risk of Infection: Smaller incisions may lead to a decreased risk of infection and less blood loss.
Disadvantages of Laparoscopic Surgery
- Skill Requirement: Laparoscopic surgery demands specialized training and expertise, and not all surgeons are proficient in this technique.
- Not Suitable for All Cases: Some complex or large hernias may be challenging to repair laparoscopically.
Choosing the Right Approach
The decision between laparoscopic and open surgery often depends on various factors such as the size and type of the hernia, the patient’s overall health, and the surgeon’s expertise. It’s crucial for individuals to discuss these options thoroughly with their healthcare provider to determine the most suitable approach for their specific situation.
Both laparoscopic and open surgery for hernia have their own set of advantages and drawbacks when it comes to hernia repair. While open surgery provides direct access and is a versatile technique, laparoscopic surgery offers a minimally invasive approach with faster recovery times.
The choice between these procedures should be carefully evaluated in consultation with a healthcare professional, ensuring the best possible outcome for the patient’s individual circumstances.
How many days rest required after laparoscopic hernia surgery?
The majority of patients, who had laparoscopic hernia surgery are able to return to work without much restrictions after three to seven days post surgery.
How many holes are in a laparoscopic hernia repair?
During laparoscopic hernia repair or keyhole surgery, the surgeon usually makes three small incisions in your abdomen instead of a single larger incision.
Which one is best out of Laparoscopic and Open surgery for hernia repair ?
Out of Laparoscopic and open surgery for hernia repair, laparascopic hernia surgery is more suitable and preferred.
What can you not do after laparoscopic hernia surgery?
Heavier exercising at the gym, running, or lifting more than 25 pounds, No hot tubs, swimming, or soaking for 2 weeks.
Eating high fat and high caloric foods with low nutritional values, such as syrup drinks, French fries, desserts, etc.